Review of the new Canadian Guideline for Physical Activity in Pregnancy 2019
The 2019 Canadian guidelines for physical activity during pregnancy were published in the British Journal of Sports Medicine in November of 2018. (The entire November issue was actually focused on the study of exercise during pregnancy, so if you want to dive in for further detail, have a look!)
These guidelines are looking at a few questions but there are two main areas of focus. (1) The safety of exercise during pregnancy. They evaluated maternal, fetal or neonatal morbidity, and fetal mortality during and following pregnancy. (2) The benefit of exercise during pregnancy. Most mothers and healthcare practitioners are well aware that exercise is an important aspect of health at all stages of life. However, pregnancy is considered a particularly crucial time due to the impact on the health of both the mother and child and due to the fact that pregnant women are often considered vulnerable. These guidelines attempt to provide a clear consensus on the benefit versus risk balance of physical activity during gestation.
And I think they did a very good job.
What I like about these recommendations
– They are evidence-based. This includes ALL reasonably available published research AND expert opinion AND patient input. The Canadian guidelines are based on a very extensive review of the literature published up to 6 January 2017 in 3 different languages, including everything except case studies. They also created a Guidelines Consensus Panel that solicited feedback from obstetric care providers, exercise professionals, researchers, policy organizations, and pregnant and postpartum women. This is an important and often neglected aspect of evidence-informed practice and I was happy to see it.
– They openly disclose the research quality and weight. I really like how they created a ranking system for the confidence that they have in each recommendation. This allows for practitioners and parents to critically analyse the recommendation based on the weight of confidence and their individual circumstance. I also find that this adds meaning to the higher weighted recommendations.
– They are realistic. The recommendations are not aggressive or evangelical or fear-based. The activity recommendations are positive and quite achievable for most mothers. When considering fatigue during the first trimester and other obstacles they recommend that women “do what they can and return when able”.
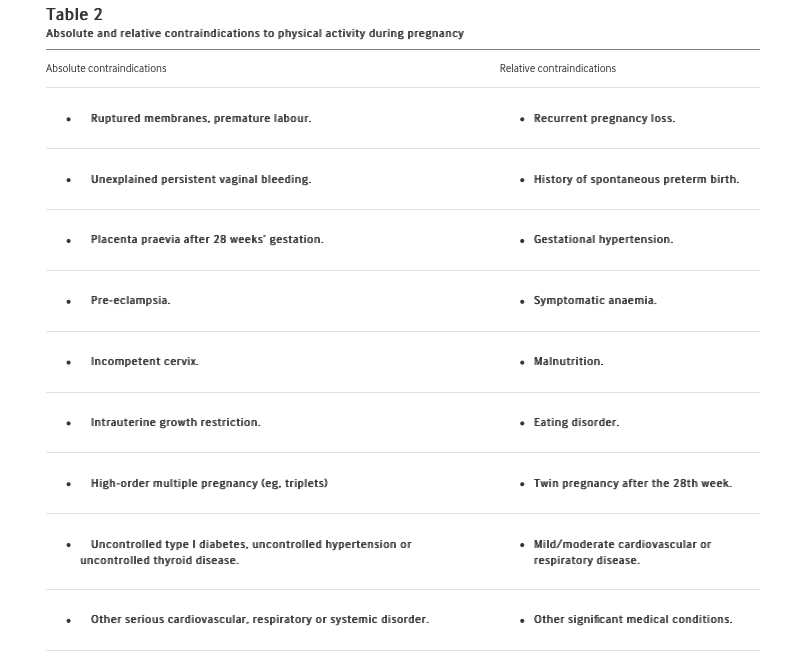

– They provided clarity in some common grey areas… mostly. We get questions so often on the contraindications to exercise during pregnancy and on which specific movements are OK or not. I appreciate the addition of Absolute and Relative Contraindications outlined in Table 2. This gives practitioners confidence in when to say a strict “no” and when to assess the situation clinically. This is a really big deal to me because we often see “bedrest” being prescribed too liberally without consideration for the physical (and mental) health impacts to the patient. In their words, “women with absolute contraindications may continue their usual activities of daily living but should not participate in more strenuous activities. Women with relative contraindications should discuss the advantages and disadvantages of moderate-to-vigorous intensity physical activity with their obstetric care provider prior to participation.”

Snowboarding at 20 Weeks Pregnant – I had to start wearing my onesie because my snow pants didn’t fit anymore.
I say mostly because in their safety precautions section they enter into the grey areas again. Their recommendations are fairly common sense when taken at face value and I understand that, from a public health perspective, it is prudent to be conservative. Saying avoid the risk of contact or falling seems obvious but where do you draw the line? I can think of moms who have safely participated in pretty much every activity listed as high risk. I know A LOT of moms who have cycled throughout their pregnancy and even one who used it as her primary mode of transportation because she does not own a car. I personally snowboarded and ran trails throughout my pregnancy and did Olympic lifting as part of my resistance training workouts until my belly got in the way of good form. You can probably also think of examples of professional, Olympic and high-level athletes completing all kinds of feats, including downhill ski racing and marathon running. I’m not saying that we should throw caution to the wind here, and I certainly would not recommend learning how to do any of these activities for the first time while pregnant. However, my husband’s aversion to fear-based decision making has worn off on me a bit in this area. I am a little more comfortable at making a case-by-case call for these sports and would also point out that there is no evidence base referenced for these recommendations; they are considered due diligence and reasonable precaution. You may need to modify, but these areas are not as black and white. In general, many women are able to continue on with activities they have enjoyed participating in, or in their words “previously active women may continue physical activity throughout pregnancy”.
I also want to highlight that moderate altitude shifts (especially under 2,500m) were given the green light (with appropriate acclimatization), since that has come up several times in office regarding heading up to hike at Big White (which is 2,315m) or elsewhere.
So on to the actual recommendations.
Conclusion: Exercise during pregnancy is beneficial and no harms were identified.
Yeah. None. Cool eh? This is a pretty big deal considering the list of benefits that were identified. Exercise during pregnancy is associated with fewer newborn complications (like being large for gestational age); decreased risk of pre-eclampsia, gestational hypertension, gestational diabetes, caesarean section, instrumental delivery, urinary incontinence, excessive gestational weight gain and depression; improved blood glucose; decreased total gestational weight gain; and decreased severity of depressive symptoms and lumbopelvic pain.
If you want some specific numbers, here they are: “Prenatal physical activity was associated with a reduction in the odds of gestational diabetes mellitus (38%; 39 fewer per thousand (from 25 fewer to 50 fewer)), pre-eclampsia (41%; 12 fewer per thousand (from 2 fewer to 19 fewer)), gestational hypertension (39%; 15 fewer per thousand (from 6 fewer to 22 fewer)), prenatal depression (67%; 134 fewer per thousand (from 90 fewer to 163 fewer)) and macrosomia (39%; 30 fewer per thousand (from 6 fewer to 47 fewer)) without increasing the odds of adverse outcomes including preterm birth, low birth weight, miscarriage and perinatal mortality.”
In terms of the benefits outweighing the risks, “physical activity is not associated with miscarriage, stillbirth, neonatal death, preterm birth, preterm/prelabour rupture of membranes, neonatal hypoglycaemia, low birth weight, birth defects, induction of labour or birth complications.”
Of particular interest, physical activity during the first trimester did not increase the odds of miscarriage or congenital anomalies. There is even evidence suggesting that not engaging in physical activity from the first trimester increased the odds of pregnancy complications (such gestational diabetes mellitus, pre-eclampsia, gestational hypertension, excessive gestational weight gain and severity of depressive symptoms).
Based on the prevalence of benefit and the lack of danger, prenatal physical activity should be considered a front-line therapy for reducing the risk of pregnancy complications and enhancing maternal physical and mental health, as well as birth outcomes.
OK. Now REALLY for the actual recommendations.
The 6 Official Recommendations for Exercise during Pregnancy
(in order of strength of recommendation)
1. All women without contraindication should be physically active throughout pregnancy.
This is broken down slightly into subgroups for which there is some direct research. Of these, previously inactive and overweight/obese mothers are considered those who will benefit the most from physical activity during pregnancy. This is not surprising. In general, as with nutrition research, those with the biggest deficit often stand to benefit the most.
2. Pregnant women should accumulate at least 150 min of moderate-intensity physical activity each week to achieve clinically meaningful health benefits and reductions in pregnancy complications.
That is equivalent to a 30-minute activity 5 days a week (in case you didn’t feel like doing the math yourself). That is the minimum. There was a dose-response relationship, meaning increasing intensity and amounts of exercise were associated with greater decreasing “odds of pre-eclampsia, gestational diabetes, gestational hypertension, and a reduction in depressive symptoms and circulating maternal blood glucose”. The more the merrier, but 150 minutes a great place to start, especially if you are previously inactive.
3. Physical activity should be accumulated over a minimum of 3 days per week; however, being active every day is encouraged.
No crazy binge exercising. Best to do something active every day.
4. Pregnant women should incorporate a variety of aerobic and resistance training activities to achieve greater benefits. Adding yoga and/or gentle stretching may also be beneficial.
In their words, “combining aerobic exercise and resistance training during pregnancy was more effective at improving health outcomes than interventions focused on aerobic exercise alone”. This is really exciting for us because, as practitioners helping mothers during this crazy time of transformation, we are usually focusing on increasing resistance training based on the direct impact managing the changing body biomechanics throughout pregnancy. Resistance training often tends to be lower impact and it is something you can do in smaller time chunks. Plus it helps your body physically strengthen in preparation for the demands of child-rearing to come.
5. Pelvic floor muscle training (PFMT) (eg, Kegel exercises) may be performed on a daily basis to reduce the risk of urinary incontinence. Instruction on the proper technique is recommended to obtain optimal benefits.
This is a cool new category. It was not considered the strongest recommendation based on the research base but I am excited to see this area being recognized in the public and scientific circles. Even though the quality of evidence is not high, “prenatal PFMT is associated with a 50% reduction in prenatal and 35% reduction in postnatal urinary incontinence”. Sold yet? I would also like to emphasize the importance of proper instruction here. It’s not so simple as being able to stop your pee mid-flow. This is a great opportunity to seek out a pelvic floor physio while pregnant (and, I would add, to follow up with them postnatal as well).
6. Pregnant women who experience light-headedness, nausea or feel unwell when they exercise flat on their back should modify their exercise position to avoid the supine position.
There was considered very weak confidence in this recommendation. Here is why that matters. So many women (and practitioners or support people) are terribly paranoid about laying flat on their backs while they are pregnant. You are safe to do so so long as you feel well while in that position; but if it unpleasant, don’t do it.
Why do the recommendations matter?
Based on the researchers, “fewer than 15% of women will actually achieve the minimum recommendation of 150 minutes per week of moderate-intensity physical activity during their pregnancy”. That is dismal. Having strong, confident, clear recommendations will help practitioners coach patients more effectively and will help parents feel safe in following practitioner encouragements.
“Concerns over harms have not been substantiated by research and the risks of not engaging in prenatal physical activity have not been adequately emphasised. Over the last three decades, the rates of pregnancy complications such as gestational diabetes mellitus, pre-eclampsia, gestational hypertension and newborn macrosomia have risen dramatically, most likely as a consequence of rising rates of maternal obesity. Physical activity has been proposed as a preventative or therapeutic measure to reduce pregnancy complications and optimise maternal-fetal health.” That is what we are all about. What is the safest, most conservative way to do the most good for mom and baby? Well, here you have it.

SUP while Pregnant – A good low intensity activity
Additional Points of Interest
Diastasis Recti (DR)
This has become quite the hot topic over the last couple of years and I am happy to see more attention being paid to postnatal rehab because of it. As with anything that becomes internet famous, there is also a fair bit of faulty information circulating. Women who begin to develop DR during pregnancy should see a maternity-based exercise-savvy physical therapist (or chiropractor) during pregnancy for direct activity advice and absolutely should followup postnatal to assure complete recovery without consequence. It is prudent to avoid flexion-based abdominal exercises (like crunches and situps) while pregnant (whereas other core exercises done properly after coaching are ok). Participating in aerobic exercise such as walking is associated with decreased odds of developing diastasis recti.
Competitive & Elite Athletes
This is an add-on to my grey area discussed above. “Women considering athletic competition or exercising significantly above the recommended guidelines should speak to their obstetric care provider to clarify risk and make modifications, if necessary. Elite athletes who continue to train during pregnancy are advised to seek supervision from an obstetric care provider.” The International Olympic Commity (IOC) actually has a 4-Part series published on exercise during pregnancy for elite athletes which goes a little more in-depth as to the physical and physiological specifics of more strenuous exercise during pregnancy. This is one of the reasons why I referred to the earlier recommendation as a grey area and these articles are a useful tool for women and practitioners to take into considerations for the more “extreme” active population.
IOC article on Exercise and pregnancy in recreational and elite athletes.
For the average “Jane” out there, the PARmed-X for Pregnancy is a tool that can be used to assess readiness for exercise if you are still feeling cautious.
Irony?
Finding it funny that the updated Canadian guidelines published in the British Journal of Sports Medicine? The British Medical Journals are considered some of the most respected in the world (or what one of my mentors Dr Monica Buerger would call “God’s Journals’). This is not a dig on any Canadian scientific journals. It just adds to the prestige and is more likely to impact international recommendations. This article was also co-published in the Journal of Obstetrics and Gynaecology Canada.
Hungry for More?
If you did not get your fill reading all of my takeaways or you want to fact-check me, you can read the full-text article yourself.
If you want more guidance on how to get started, check out this blog on Exercise During Pregnancy.
Want someone to give you more guidance on your specific situation? Book in with one of our chiropractors.
