Probiotics During Pregnancy
Let’s take a step back (from our first blog on the microbiome). What about before birth? What about during pregnancy? Of course, our dietary choices, supplements, medications, stress-load, and physical experiences all impact both mom and baby in-utero. The womb is not quite the sterile environment we once thought it was. There is a growing body of evidence demonstrating direct in-utero transfer of microbiota from the placenta and amniotic fluid to the fetus. We know that certain nutrient deficiencies and exposures to teratogens during pregnancy result in both predictable and unknown insults to a developing fetus, from folate-deficient neural tube defects to thalidomide-induced phocomelia. I prognosticate that over the next few years, we will discern a more predictable pattern of the impacts of maternal dysbiosis on her child’s health but, for now, it is a dynamic exploration of terra incognita and we need to make the best evidence-informed decisions we can as parents and practitioners, which sometimes means not waiting for the research to catch up.

First, do no harm. Of all the thousands of research articles out there in one of the fastest growing areas of medicine, one key takeaway is that probiotic supplementation is very safe in pregnancy. This does not mean that there are no repercussions for error but does give a buffer of not having to be “up on the latest” to make a good, helpful recommendation. We have also come a very far way from the basic “eat some yoghurt”. {Side Story: I had an MD a couple years ago tell me that there was this “new thing called kefir” out there now that I should take with antibiotics. I giggled to myself and said thank you. He was doing the best with what he knew at the time!} Saying “take a probiotic” is no longer enough. With strain-specificity and clinical dosage, we have exponentially more success.
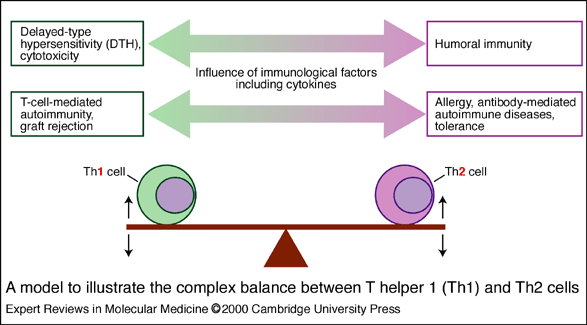
We not just talking about how to rehabilitate damage done from antibiotics taken during pregnancy. That is absolutely important. However, we can now go step further to supporting a healthy microbiome to enhance the health of our offspring. Mom supplementing with specific strains of probiotics during pregnancy (especially during the third trimester) will help colonize her newborn’s GI tract with a more ideal initial blend of bacteria. This is a REALLY big deal (which we will explore more in detail in another upcoming blog). The initial microbiota that a baby is exposed to play an important role in preparing the environment for a healthy, diverse microbiome in the coming months. They improve digestion and food tolerance. They are also crucial for the early education of the developing immune system (in particular, recognizing and regulating self versus non-self and Th1/Th2 balance for my biochem mom-dorks out there who were wondering).
Oral probiotics have also been shown to restore normal vaginal flora in women with bacterial vaginosis and there is good evidence to support their usage for reducing the risk of GBS. This is obviously important for the infant’s initial seeding exposure but studies are even starting to show that dysbiosis may impact birth outcomes. There is an association between microbial imbalance and premature rupture of membranes, preterm delivery, and low infant birth weight, all of which come with their own bag of troublesome worms.
So which probiotics should you take? A probiotic containing a high-dose of Lactobacillus rhamnosus is a good place to start; this strain is supportive of mom’s vaginal health and, when taken during pregnancy and continued on for the first 6 months, can decrease the risk of eczema by about 50%.
A Summary of Probiotics During Pregnancy
- Baby’s health outcomes are impacted by mom’s microbiome and her choices/exposures during pregnancy.
- Nutrition and supplementation recommendations, including probiotic strains and doses, should be specific to the microbial imbalance being addressed.
- Supporting a healthy microbiome during pregnancy can help reduce GBS risk and bacterial vaginosis.
- This includes a healthy diet high in vegetable fibre and polyunsaturated fats and low in sugar, as well as reducing your stress load and taking a “women’s” probiotic.
- Taking certain probiotics during pregnancy may reduce the risk of atopic diseases (eczema, asthma, allergies) in infants.
A Note on What Is Not Being Discussed
To discuss the fields not being discussed seems odd, but I wanted to touch on the fact that there are so many other relevant conditions during pregnancy and health concepts pertinent to mother and child that are being studied extensively regarding their relationship to the microbiome. Among the more prevalent are the association between dysbiosis and obesity, gestational diabetes, preterm labour, hypertension and preeclampsia, low birth weight, and mastitis. I would love to explore each of these independently – for my own edification and for your sake – but I needed to focus in on the heavy hitters in order to maintain some semblance of a life outside my dorky deep-dives down the academic rabbit hole.
References
- Collado M et al. Human gut colonisation may be initiated in utero by distinct microbial communities in the placenta and amniotic fluid. Scientific Reports 2016; 6(23129).
- Doege et al. Impact of maternal supplementation with probiotics during pregnancy on atopic eczema in childhood – a meta-analysis. British Journal of Nutrition 2012; 107: 1–6.
- Dotterud CK, Storrø O, Johnsen R, Øien T. Probiotics in pregnant women to prevent allergic disease: a randomized, double-blind trial. British Journal of Dermatology 2010; 163:616-623.
- Elazab N et al. Probiotic Administration in Early Life, Atopy, and Asthma: A Meta-analysis of Clinical Trials. Pediatrics 2013;132:e666–e676.
- Huurre A et al. Impact of maternal atopy and probiotic supplementation during pregnancy on infant sensitization: a double‐blind placebo‐controlled study. Clin Ex Al 2008; 38(8):1342-1348.
- Jacobsson B, Pernevi P, Chidekel L, Platz-Christensen J. Bacterial vaginosis in early pregnancy may predispose for preterm birth & postpartum endometritis. Acta Obstet Gynecol Scand 2002; 81:1006-10.
- Kalliomäki M et al. Probiotics in the prevention of atopic disease: a randomised placebo-controlled trial. Lancet 2001; 357:1076-9.
- Kalliomäki M et al. Probiotics and the prevention of atopic disease: 4-year follow-up of a randomised placebo-controlled trial. Lancet 2003; 361:1869-71.
- Kidd P. Th1/Th2 Balance: The Hypothesis, its Limitations, and Implications for Health and Disease. Altern Med Rev 2003; 8(3):223-246.
- Kukkonen K et al. Probiotics and prebiotic galactooligosaccharides in the prevention of allergic diseases: A randomized, double-blind, placebo-controlled trial. J Allergy Clin Immunol 2007;119:192-8.
- Pelucchi C et al. Probiotics Supplementation During Pregnancy or Infancy for the Prevention of Atopic Dermatitis: A Meta-analysis. Epidemiology 2012; 23(3): 402-414.
- Purwar M, Ughade S, Bhagat B, Agarwal V, Kulkarni H. Bacterial vaginosis in early pregnancy and adverse pregnancy outcome. J Obstet Gynaecol Res 2001; 27:175-81.
- Rautava S, Kalliomäki M, Isolauri E. Probiotics during pregnancy and breastfeeding might confer immunomodulatory protection against atopic disease in the infant. J Allergy Clin Immunol 2002;109:119-21.
- Rautava S, Kainonen E, Salminen S, Isolauri E. Maternal probiotic supplementation during pregnancy and breastfeeding reduces the risk of eczema in the infant. JACI 2012; 130(6):1355–1360.
- Reid G, Beuerman D, Heinemann C, Bruce AW. Probiotic Lactobacillus dose required to restore and maintain a normal vaginal flora. RFEMS Immunol Med Microbiol 2001; 32:37-41.
- Reid G, Hammond JA, Bruce AW. Effect of lactobacilli oral supplement on the vaginal flora of antibiotic-treated patients: randomized, placebo-controlled study. Nutraceut Food 2003; 8:145-8.
- Schultz M, Gottl C, Young RJ, Iwen P, Vanderhoof JA. Administration of oral probiotic bacteria to pregnant women causes temporary infantile colonization. J Pediatr Gastroenterol Nutr 2004; 38:293-7.
- Sult T. Th1/Th2 Balance: A Natural Therapeutic Approach to Th2 Polarization in Allergy. ANSR 2003; 676.
